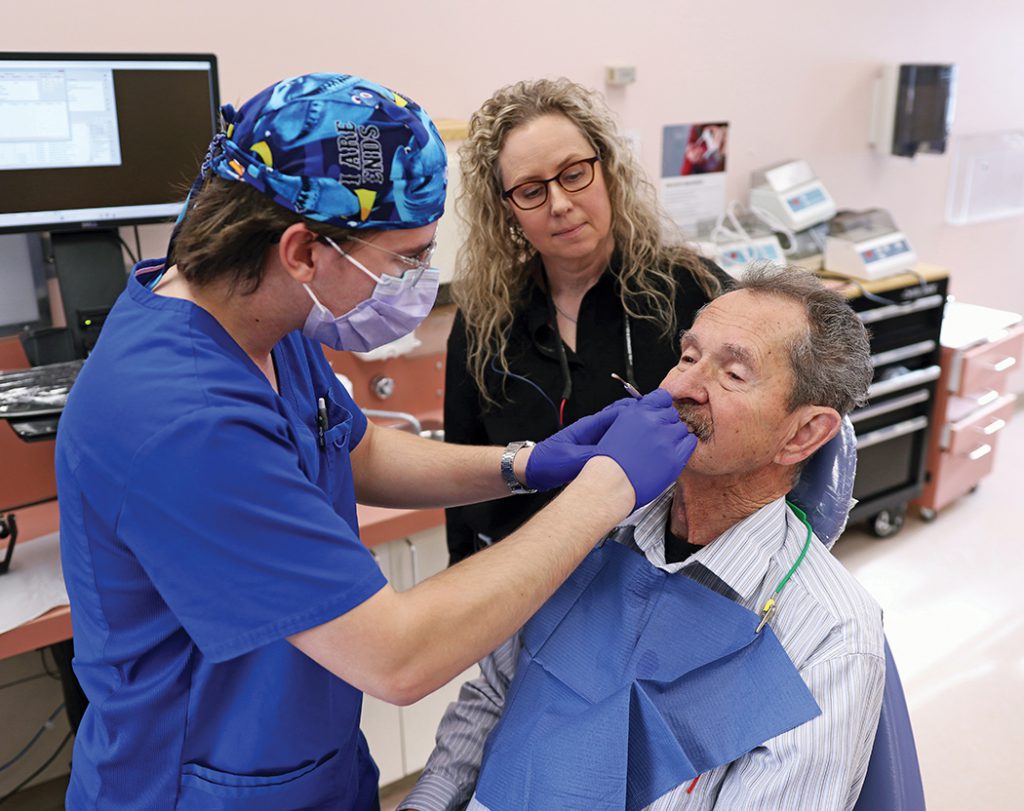
The Dr. Gerald Niznick College of Dentistry has received more than $6.1 million in federal funding to improve access to care for underserved populations and expand learners’ experience in caring for these patients.
The financial support for four UM projects is provided through Health Canada’s Oral Health Access Fund (OHAF).
The fund has invested a total of $35 million in 30 initiatives at dental schools across Canada.
“It’s a win-win for people in need, and for our learners,” says Anastasia Kelekis-Cholakis [DMD/92, Dip.Perio/98], dean of the dental college.
“This academic year at our general clinic, we’ve been able to cover the full cost of eligible care for many patients who don’t have private dental insurance and face socio-economic barriers to obtaining care.”
The funding has also greatly benefited students, the dean says, because it has attracted a new pool of patients. “In order for our dentistry and dental hygiene students to complete all the hands-on training they require to graduate, we need a consistent flow of patients who require a variety of procedures,” she says.
While serving as chair of the Association of Canadian Faculties of Dentistry, Kelekis-Cholakis took a leadership role in advocating for the creation of the Oral Health Access Fund.
The fund complements the Canadian Dental Care Plan (CDCP), the recently introduced government dental insurance program that provides coverage for uninsured people with incomes below certain thresholds.
“We knew that the CDCP would divert patients away from university teaching clinics because many Canadians who used to go to dental schools to save money can now use their CDCP coverage at private dental practices,” Kelekis-Cholakis says.
The OHAF support is enabling UM to retain some CDCP patients by covering their co-payments, she says.
It is also extending care to people with low incomes who are not enrolled in the CDCP for reasons such as being new to Canada, not filing a tax return, facing literacy barriers, being unhoused, or lacking the means to afford any co-payment or other fee.
Three of the UM projects involve clinical care, while the fourth is an educational initiative. Kelekis-Cholakis hopes to see all three clinical projects sustained through permanent funding.
“The impact has been transformational,” she says. “We’re advocating for the federal government to continue the support. It’s crucial to the education of the oral health-care workforce, and to serving our community.”
Attracting and retaining patients from priority populations
The dental college received $336,000 to cover up to 100 per cent of eligible care at the college’s general clinic for patients who are enrolled in the CDCP or are uninsured. Care will be fully covered until March 31, 2026.

Taking this approach since September 2025 has brought in a large influx of patients with significant needs, says project lead Dr. Trenna Reeve, associate dean (clinical).
“I told the students, ‘Let’s make an impact on people’s lives,’” Reeve says. “By mid-December, we had allocated more than $240,000 of the funding to patient care.
“We’re treating seniors, Indigenous people, people with insecure housing, people with disabilities. The large majority have not had treatment for 10-plus years.”
Fourth-year student Costa Papasotiriou says in past years at the school, many patients could only afford a small fraction of the dental work they needed.
“This fund has allowed these patients to get comprehensive care because their entire treatment plan is covered. For students, it has allowed us to get a lot more experience.”
The students are developing important skills in treating at-risk patients with dignity and compassion, Reeve says.
Papasotiriou says he felt great about helping Wayne, a 79-year-old patient who had glued his broken dentures together because he couldn’t afford new ones. Thanks to the OHAF funding, Wayne received new dentures at no cost.
Training professionals in community oral health
The college received $1.8 million to pilot, for three years, a 12-month postgraduate apprenticeship program in community oral health and dental public health.
This funding has enabled a dentist and two dental hygienists – recent UM grads – to work since August 2025 as paid apprentices with UM’s Centre for Community Oral Health (CCOH).
The CCOH operates clinics at Winnipeg sites including Access Downtown and Deer Lodge Centre, as well as a mobile program that serves personal care homes. The OHAF support has funded equipment upgrades and allowed more patients to access care, says project lead Robert Schroth [DMD/96, M.Sc./03, PhD/10], director of the CCOH.
There’s an ongoing shortage of oral health professionals who choose to practise in community-based programs in Manitoba, Schroth says.
“This program is developing the apprentices’ skills, interest and knowledge. We hope they’re inspired to specialize in public health, or to continue devoting some of their clinical time to priority populations.”
Each apprentice will also complete a scholarly project to broaden their understanding of oral health science.
Building community ties for better oral health
The School of Dental Hygiene was awarded OHAF funding of $344,740 to pilot an oral health community liaison role.
Two dental hygienists have been employed since September 2025 in this outreach role. They are strengthening UM partnerships with organizations such as Main Street Project, Siloam Mission and 1JustCity that serve people in need, including Indigenous people and refugees.
The liaisons give presentations about oral health and perform oral screenings at community sites. They refer patients to the UM campus clinic, or to other clinics if appropriate. Patients receive personalized help with understanding their eligibility, completing their paperwork, and with transportation.
“Past trauma, anxiety and not knowing what to expect are barriers to people accessing care,” says project lead Mary Bertone [Dip.D.Hyg./05, B.Sc.D.Hyg./11, MPH/15], director of the School of Dental Hygiene. “We’re supporting individuals in the journey to come and receive person-centred care.”
Future dental hygienists and dentists are learning from these patients how to understand people’s challenges, respond with empathy and provide culturally safe care, Bertone adds.
Educational modules for oral health-care learners
The college received $3.6 million to lead a national team in creating 10 online learning modules. The goal is to better prepare oral-health professionals to deliver appropriate, person-centred care to members of groups that experience inequitable access.
Experts from Canada’s 10 dental schools and stakeholders from the priority groups will collaborate on the educational content.
The modules, which will be provided on the Association of Canadian Faculties of Dentistry’s website, are intended for both dental-school curriculum and professional development use.
UM will contribute expertise on delivering culturally competent care to Indigenous patients. Chantal Daniels, director of Ongomiizwin – Education in the Rady Faculty of Health Sciences, is part of the team developing the Indigenous module.
She wants every oral-health professional to understand the effects of colonization on Indigenous health; how care is funded for Indigenous patients; and that Indigenous Peoples have traditional knowledge for oral health.
“We have had oral care for millennia,” Daniels says.
Read more about the Oral Health Access Fund projects.
BY ALISON MAYES
